Torres Strait Islanders have among the highest prevalence of diabetes in Australia. Glycaemic control is a challenge in the Torres Strait Islands and rates of insulin treatment are low.
Complications from diabetes are common and include renal failure, vision loss, lower limb amputation, and even death.
Diabetes is recognised as a major health challenge facing Australia’s Indigenous peoples. Prevalence rates are 3 to 4 times the non-Indigenous rate, across all age groups. It is the second leading underlying cause of death of Indigenous people, and the leading cause of death among Indigenous women.1
There are opportunities for specialists to help close this important part of the Indigenous health and life expectancy gap. Remote areas, like the Torres Strait Islands, need specialists. In 2012–13, diabetes was almost twice as prevalent among Indigenous adults living in remote areas than among those living in non-remote areas.2
Snapshot | Torres Strait Islands and Islanders
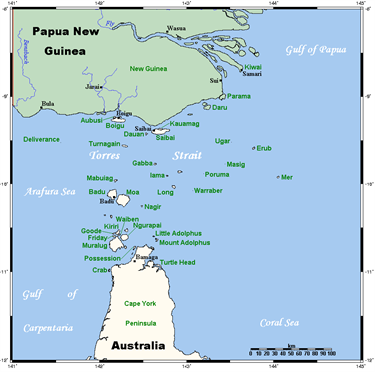 The 274 islands at the tip of Cape York are about 800 km from Cairns. Most were annexed by Queensland in 1879, with a few administered from Papua New Guinea.
The 274 islands at the tip of Cape York are about 800 km from Cairns. Most were annexed by Queensland in 1879, with a few administered from Papua New Guinea.
Islanders comprise five cultural groups that are distinct from Aboriginal peoples. They practise hunting, fishing and agriculture. Two main traditional languages and six dialects are spoken, as is Kriol – a mix of traditional languages and English.
Most Islanders now live on the mainland, but 17 islands with permanent fresh water are inhabited by about 6500 people, the majority Indigenous. Thursday Island, the islands’ administrative centre, is only 3.5 km2 but has a population of about 3000 people. Most islands have between 100 and 200 inhabitants.
Primary Health Care Services
Culturally Appropriate Primary Health Care
Queensland Health’s Torres and Cape Hospital and Health Service (TCHHS) is responsible for the Thursday Island Primary Health Care Centre which opened in 1997 and acts as a hub for 15 other primary health care centres across the islands. Most of these comprise a remote nurse, Indigenous Health Workers and ancillary staff supported by telehealth. Outreach GP services have been operating for over twenty years and also can work from these clinics. All the islands’ primary health centres operate under a model of care that supports Indigenous management and culturally appropriate health services. TCHHS also operates a 32-bed referral hospital and a rehabilitation centre on Thursday Island. Travel assistance to other Queensland hospitals is available for patients.
Diabetes Care
Thursday Island Primary Health Care Centre acts as a hub for diabetes services, with GPs based there running a diabetes clinics and managing patients in the other islands via telehealth and outreach. These are coordinated by the smaller island primary health centres with Indigenous Health Workers playing a critical liaison role with patients, as well as in ongoing patient follow up and monitoring.
Case study | Thursday Island Primary Health Care Centre Diabetes Clinic
“Patients avoiding the stress, costs and time associated with often very long-distance and difficult travel are a quality saving that you can’t measure”
– Dr Ashim Sinha
Endocrinologist Dr Ashim Sinha is based in Cairns Hospital and is a team member of the Thursday Island Primary Healthcare Centre. He works in partnership with multidisciplinary primary health care teams including nurses, GPs, Indigenous Health Workers, and Diabetes Educators who work with families and communities on the Torres Strait Islands.
He does this by:
- working on site at the Thursday Island Primary Healthcare Centre Diabetes Clinic on a regular basis with the team there, particularly to see patients with complex presentations. This is reached by one of the two daily flights from Cairns to Horn Island, where the airport is an 8km ferry journey from Thursday Island.
- conducting weekly telehealth consultations. These may include patient consultations but also allow a time for Dr Sinha to discuss cases with primary health care teams and to provide them with ongoing education, building capacity in diabetes-related primary health care on the islands.
"Working with specialists empowers primary health care teams to provide more than band aid solutions and be involved in broader aspects of the health system"
– Maggie, Diabetes Educator
The Principles in Action: What Makes Dr Sinha’s Outreach Work?
Indigenous leadership
Indigenous leadership occurs through specialists working with and in Torres Strait Island primary health care centres under a model of care that supports Indigenous management of health services and the cultural safety and appropriateness of services. Different models of outreach can be implemented depending on an island’s needs and circumstances.
Culturally safe
- Working with Indigenous Health Workers who can also act as cultural brokers, even translators, for patients. Dr Sinha acknowledges the vital role played by Indigenous Health Workers prior to, during and after his consultations, and, whenever possible, aims to have an Indigenous Health Worker present during consultations.
- Long-established relationships with communities enable specialists to better understand and work with cultural differences over time. A cultural protocols committee in the Torres Strait influenced the development of this model.
A one-year randomised cluster trial in the Torres Strait showed reduced hospital admissions and improved care processes when local Indigenous health workers were supported by outreach specialist services to provide basic diabetes care plans and patient recalls. A three year follow up clinical audit showed that clinical improvements remained two years after the trial.
Person-centered and family-orientated
- Outreach services enable patients to access care in their own community without them having to leave country, family and community support.
- Family members will often be involved in patient consultations, recognising the importance of family support and involvement in health care. Sometimes other family members are involved in shopping and meal preparation, a whole of family approach can assist with lifestyle changes.
Flexibility
Telehealth consultations enable flexibility – Dr Sinha can hold an urgent consultation from Cairns with two hours’ notice, in addition to routinely scheduled telehealth.
Sustainable and feasible
- Institutional culture – Diabetes is a priority health area for Cairns Hospital. Further, outreach - including to the Torres Strait, is viewed as ‘core business’ of the Cairns Hospital-employed specialists, and they are encouraged, and released, to undertake such.
- Funding and administrative support – MBS items are used for patient consultations and the Rural Health Outreach Fund covers the costs of specialist travel and accommodation. However, billing is a complex, time consuming task which requires the attention of a full-time staff member to ensure that all claims are made. Without this, outreach services would not be financially viable for Cairns Hospital.
- Team work – Collaboration and communication with primary care staff including by case conferencing helps ensure holistic patient care and that Dr Sinha consults only with patients in need of specialist services, and not those that can be managed in primary care centres.
Building Capacity in the Health System
Outside of the Torres Strait, Dr Sinha also participates in a ‘Physician in Practice’ model of care at Mulungu Aboriginal Corporation in Mareeba, a one hour drive from Cairns. This involves joint specialist-GP consultations which benefit patients and provides GP education. It also helps build trust between GPs and specialists, and between specialists and patients
Integration and continuity of care
- Information sharing – outreach is of limited use if patient information gleaned is not available to health workers at other points of a patient’s treatment journey. Because of Cairns Hospital’s support for outreach, and its capacity to hold patient data gleaned through outreach in a central place, this risk is minimised.
- Building relationships with patients, families and communities – Dr Sinha believes building long-term health care service and professional - patient relationships are key to success in outreach work, and can start with GP training. In this way, a GP can get to know families and communities over time and build trust with them, and this in turn facilitates their building trusts with specialists introduced to them.
- Continuity of care – when an outreach patient needs to receive treatment at Cairns Hospital, services try to match staff they are already familiar with through outreach activities to their care. This is to ensure a ‘familiar face’ is present, and otherwise assist them and medical staff if required.
Download PDF
Read next: Marrabinya: Aboriginal Health in Aboriginal Hands